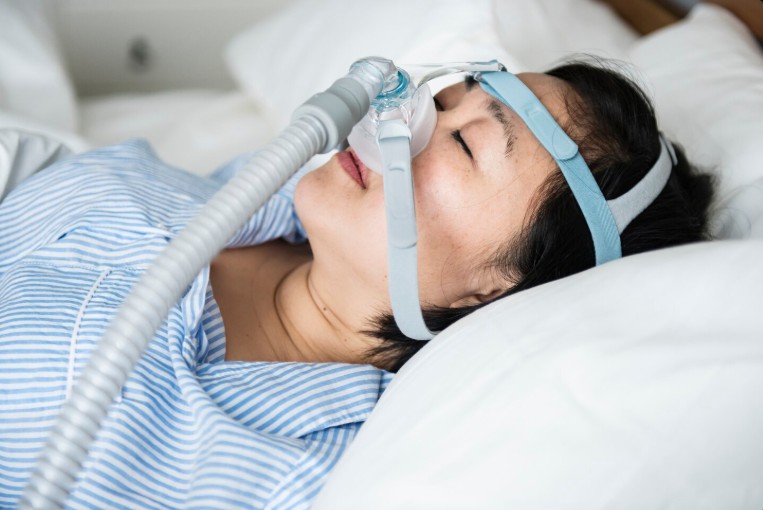
This article is for every person who snores, every partner who lies awake listening to it, and every patient who wakes up tired no matter how many hours they sleep. In this article, Dr. Shivanshu Raj Goyal, sleep disordered breathing specialist in Gurgaon, explains what’s really happening while you sleep.
Sleep disordered breathing is an umbrella term that covers a spectrum of conditions — from simple snoring at one end, to Obstructive Sleep Apnoea (OSA) and Obesity Hypoventilation Syndrome at the other.
Obstructive sleep apnoea is the most common type of sleep disordered breathing, characterized by recurrent episodes of upper airway collapse during sleep — causing repeated, complete or partial cessation of airflow, despite continued breathing effort.
In plain language: your airway collapses while you sleep. You stop breathing. Your body panics, partially wakes you up to restart breathing, and then you fall back asleep — often with no memory of it. These pauses in breathing can last from a few seconds to minutes and may occur 30 times or more in a single hour.
You wake up in the morning feeling like you haven’t slept at all. Because, in a very real sense, you haven’t.
The Symptoms You’re Probably Ignoring
Frequent loud snoring, witnessed breathing pauses during sleep, restless sleep, waking up to urinate repeatedly at night, and mouth breathing are hallmark features of sleep disordered breathing.
But the symptoms that bring most patients to my clinic are the daytime ones — and they are often misattributed to stress, depression, or simply working too hard:
Waking up exhausted despite 7 or 8 hours in bed. Sleep is supposed to restore you. If it isn’t, something is disrupting it repeatedly through the night.
Falling asleep at your desk, in meetings, or while driving. This is not laziness. Excessive daytime sleepiness is one of the most debilitating consequences of obstructive sleep apnoea, significantly impairing work performance, cognitive function, and quality of life.
Morning headaches. The result of repeated drops in oxygen levels through the night.
Mood changes, irritability, and difficulty concentrating. Many patients with undiagnosed sleep apnoea are first treated for depression or anxiety — when the real problem is they have never had a night of proper, restorative sleep.
High blood pressure that won’t come down despite medication. This is one of the most significant and underappreciated connections in all of medicine.
Why This Is a Medical Emergency — Not a Lifestyle Inconvenience
This is the part where I need you to sit up and pay attention.
Obstructive sleep apnoea is one of the most serious sleep disorders because of repeated cycles of upper airway collapse during sleep, resulting in intermittent hypoxia, sleep fragmentation, and excessive daytime sleepiness — and it is strongly associated with cardiovascular disease, metabolic disorders, and neurocognitive impairment.
Every time sleep apnoea causes a breathing pause, it triggers a spike in blood sugar, heart rate, blood pressure, and stress hormones — a stress response similar to what you might experience being asked to speak in front of a large crowd. Imagine that happening 30 or 40 times every single night.
Over months and years, this relentless nightly stress response causes:
- Hypertension — blood pressure that is elevated from the moment you wake up
- Increased risk of heart attack and stroke
- Type 2 diabetes — repeated oxygen drops impair insulin sensitivity
- Atrial fibrillation — irregular heart rhythm with serious complications
- Road traffic accidents — drowsy driving is as dangerous as drunk driving
Long-term treatment with CPAP therapy has been shown to reduce both mortality and the acute blood pressure elevation that occurs with sleep disordered breathing. The condition is treatable. The damage, if left long enough, is not always reversible.
Who Is at Risk?
Sleep disordered breathing does not discriminate — but certain factors significantly increase your risk:
Excess weight — fat deposits around the neck narrow the airway. Sleep apnoea occurs in about 3% of normal-weight individuals but affects over 20% of obese people.
Being male — men are more commonly affected, though the gap narrows significantly after menopause in women.
Gurgaon’s corporate lifestyle — late nights, high stress, sedentary work, irregular eating, and weight gain create the perfect storm for sleep disordered breathing to develop and go undetected.
A thick neck, small jaw, or large tonsils — structural factors that narrow the upper airway during sleep.
Alcohol before bed — alcohol relaxes the throat muscles further, worsening airway collapse.
How Is It Diagnosed?
A sleep specialist can order a sleep apnoea test — using equipment to monitor your breathing and oxygen levels while you sleep. This can be done in a sleep laboratory overnight, or with a portable take-home kit. undergo a home sleep study — a convenient, accurate test done in the comfort of your own bed. For more complex cases, a full overnight polysomnography in a sleep laboratory gives us the most detailed picture.
The Apnoea-Hypopnoea Index (AHI) tells us how many times per hour your breathing is disrupted. Severe obstructive sleep apnoea means your AHI is greater than 30 — more than 30 breathing disruptions per hour. I have seen patients come in at 60, 70, even higher — having no idea their sleep was this severely fragmented.
Treatment: What Actually Works
The good news is that sleep disordered breathing responds very well to the right treatment.
CPAP Therapy remains the gold standard. Continuous positive airway pressure therapy remains the gold standard treatment for sleep disordered breathing, and is highly effective in improving sleep quality and reducing daytime sleepiness — with newer therapies including mandibular advancement devices and hypoglossal nerve stimulation also becoming available.
Most patients who commit to CPAP therapy notice a dramatic difference within the first few nights — waking up genuinely refreshed for the first time in years.
BiPAP Therapy for patients who cannot tolerate standard CPAP, particularly those with more complex breathing patterns or severe disease.
Oral appliances — custom-fitted devices that hold the jaw forward and keep the airway open, suitable for mild to moderate cases.
Weight loss — even a modest reduction in weight can significantly improve airway patency and reduce AHI.
Lifestyle modifications — sleeping on your side, reducing alcohol, and treating nasal congestion all contribute meaningfully to improvement.
Surgery — considered in specific structural cases after thorough evaluation.
A Word on Women and Sleep Apnoea
Women are significantly underdiagnosed with this condition — and it is not because they have it less. It is because their symptoms present differently. Rather than loud snoring and witnessed apnoeas, women more often report insomnia, fatigue, morning headaches, and low mood. These get attributed to hormones, stress, or anxiety — and the underlying sleep disordered breathing goes uninvestigated for years.
If you are a woman and this article resonates with you — please don’t assume this condition doesn’t apply to you.
FAQs: Sleep Disordered Breathing — Dr. Shivanshu Raj Goyal Answers
Q1. Is snoring always a sign of sleep disordered breathing?
Not always — but it is always worth taking seriously. Simple snoring without breathing pauses may be harmless. However, loud, disruptive snoring — especially when accompanied by witnessed pauses in breathing, gasping, or daytime exhaustion — is a strong indicator of obstructive sleep apnoea and should be properly evaluated. A history of disruptive snoring combined with witnessed breathing pauses has a 94% specificity for sleep disordered breathing.
Q2. Can I do a sleep study at home or do I need to come to a hospital?
Most patients can be accurately diagnosed with a home sleep apnoea test — a small, comfortable device worn overnight that monitors your breathing, oxygen levels, and heart rate while you sleep in your own bed. For patients with complex symptoms or suspected non-obstructive causes, a full in-laboratory polysomnography may be recommended for a more detailed assessment.
Q3. Is CPAP therapy comfortable? I’ve heard people can’t tolerate it.
CPAP technology has improved dramatically in recent years. Modern CPAP machines are quiet, compact, and highly adjustable. There is a short adaptation period, but the vast majority of patients who persist with CPAP for two to four weeks find it genuinely comfortable — and transformative in terms of how they feel. I work closely with every patient to find the right mask fit and pressure settings, because CPAP done right changes lives.
Q4. Can sleep disordered breathing cause high blood pressure?
Absolutely — and this is one of the most important connections in medicine that is still widely underappreciated. Long-term CPAP treatment reduces both mortality and the acute blood pressure elevation that occurs with sleep disordered breathing. Many patients find their blood pressure improves significantly after starting CPAP — sometimes enough to reduce or stop blood pressure medication entirely.
Q5. My wife says I stop breathing in my sleep — but I feel fine during the day. Do I still need to be seen?
Yes — urgently. Witnessed apnoeas during sleep are one of the most reliable indicators of significant obstructive sleep apnoea. The fact that you feel fine during the day may simply mean you have adapted to a chronically sleep-deprived, oxygen-deficient baseline. Your body has adjusted to feeling less than its best, and you no longer recognize it. The cardiovascular damage, however, continues regardless of how you feel.
Q6. Can children have sleep disordered breathing?
Yes — and it is more common than most parents realize. In children, the signs are different: mouth breathing, bedwetting, poor concentration, behavioral problems at school, and restless sleep. Enlarged tonsils or adenoids are a frequent cause. If your child snores regularly or seems unusually tired or hyperactive, a sleep evaluation is worthwhile.
Q7. Why should I see Dr. Shivanshu Raj Goyal for sleep disordered breathing in Gurgaon?
As a dedicated sleep disordered breathing specialist in Gurgaon, I offer a complete pathway from evaluation to treatment — including home sleep studies, in-lab polysomnography, CPAP and BiPAP initiation and follow-up, oral appliance referral, and long-term monitoring. I take the time to understand each patient’s lifestyle, symptoms, and concerns — because the best treatment is the one you will actually use, consistently and comfortably.
Book a Sleep Evaluation with Dr. Shivanshu Raj Goyal
If you snore, if you wake up exhausted, if your partner lies awake listening to you stop breathing — please don’t wait. A sleep study is simple, non-invasive, and could be one of the most important things you ever do for your health.
A good night’s sleep is not a luxury. It is medicine. Let’s get you back to it.